 8 Interestingly, out-of-hospital cardiac arrest (OHCA) patients who had an initial non-shockable rhythm but converted to a shockable rhythm during resuscitation, had over a three-fold increase in survival rates and higher rates of good neurological outcomes. 1,3,6,7 Researchers have also shown that delays in time to defibrillation is associated with worse outcomes. Numerous studies have shown that survival rates and survival with good neurologic function have increased over time as public access to and education about AEDs has increased. Defibrillation sends an electrical current through the heart muscle cells, momentarily interrupting the abnormal electrical energy and allowing the intrinsic rhythm to resume. While chest compressions are usually just a bridge to therapy, defibrillation is the only definitive treatment for ventricular fibrillation and ventricular tachycardia. PRIORITY #2: EARLY DEFIBRILLATION WHEN APPROPRIATE The second most important intervention you can provide for your patient is early defibrillation when indicated. Consider pre-charging the defibrillator before your pulse check so that you can avoid a second pause in compressions for delivery of the shock. Remember, there is no harm to doing a few more chest compressions before stopping for a rhythm/pulse check. You can also use this delay to ensure that an ultrasound probe is in the appropriate position to view the heart during the pulse check. Consider telling the compressor to only stop when the team leader tells them to, not when the recorder/timer calls “Pulse check!” This way, you can ensure somebody has a finger on an artery to check a pulse before compressions stop, thus minimizing the time it takes to identify that there is no pulse and resume CPR. To master the art of improving the chest compression fraction, find ways to decrease pauses in compressions. It is your responsibility, as the resuscitationist, to ensure that HQ CC continue with minimal interruptions. they want to help someone place patches on the chest, they thought they heard someone tell them to stop, etc.). Paramedics, nursing assistants, and even cardiologists will frequently stop compressions for a variety of reasons (e.g. 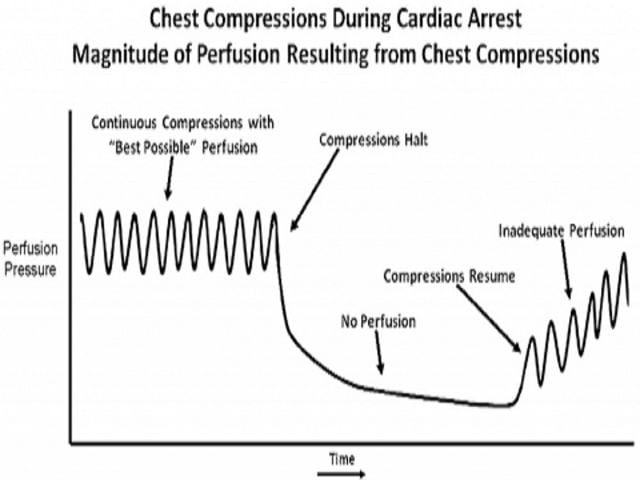 
1,2,3,4 This seems to be the best kept secret in all of medicine that only the true resuscitationists (ED and ICU nurses included) know. The one intervention that has consistently been shown to improve outcomes is early, high-quality chest compressions (HQ CC) with minimal interruptions. Controlling the room and sending out people who don’t need to be there will greatly improve the flow of the rest of the resuscitation. Tell your team ahead of time if you are considering advanced CPR practices such as pre-charging the defibrillator, infusing epinephrine instead of using bolus doses, dual sequential defibrillation, or using ETCO 2 to determine ROSC or futility.įor in-hospital cardiac arrests (IHCA), you may only have enough time to assign roles and verbalize a brief plan, but this should occur only after Priority #1 and Priority #2 have been addressed. This allows the team to have a shared mental model, so it can operate as one unit during the first part of the patient’s care. Establish and communicate a tentative plan with your team for the first few minutes of the resuscitation, with the understanding that it may change the minute your patient is wheeled through the door. during rhythm/pulse checks)ĭiscuss all the information you currently know about the patient with the rest of the team. vitals, monitor, and defibrillator manager (can also switch with compressor, but more challenging because defibrillation and compressor swaps will usually take place at the same time, i.e.  
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
